What Is a Subdural Hematoma?
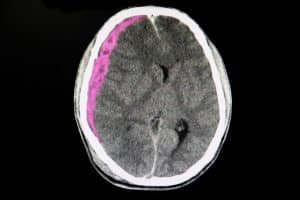
Because of the gradual onset of symptoms – and the potential for delayed diagnosis – subdural hematomas are a particularly risky injury. Understanding the dangers associated with this condition is critical for prompt diagnosis and intervention to mitigate any potential long-term neurological effects.
Per MedLine Plus, a subdural hematoma is “most often the result of a severe head injury. This type of subdural hematoma is among the deadliest of all head injuries. The bleeding fills the brain area very rapidly, compressing brain tissue. This often results in brain injury and may lead to death.”
They go on to note that “With any subdural hematoma, tiny veins between the surface of the brain and its outer covering (the dura) stretch and tear, allowing blood to collect…Some subdural hematomas occur without cause (spontaneously).”
What are the symptoms of a subdural hematoma?
Symptoms of this traumatic brain injury include headaches that progressively get worse, confusion, slurred speech, dizziness, nausea, and vomiting. Individuals may also experience changes in behavior, lethargy, and difficulty balancing. Severe cases can lead to unconsciousness, seizures, or coma.
The symptoms of a subdural hematoma can vary depending on the size of the blood clot and the rate at which it develops. In some cases, symptoms may not appear immediately after the injury. It’s essential to recognize these symptoms, especially after a head injury, as prompt medical attention is vital for properly diagnosing and treating subdural hematomas to prevent potential complications and long-term neurological damage. If any of these symptoms are present in you or your loved one, seek medical assistance immediately.
How are subdural hematomas diagnosed?
Diagnosing a subdural hematoma typically involves a combination of medical history assessment, physical examination, and imaging studies.
First, a physician will take a full medical assessment. They will inquire about the patient’s symptoms, medical history, and any recent head injuries. A thorough physical examination should be conducted to assess neurological function, including reflexes, muscle strength, and coordination.
Next, the doctor will order imaging studies, including:
- CT scan (computed tomography): This is a key diagnostic tool. A CT scan can provide detailed images of the brain and help identify the presence, size, and location of a subdural hematoma.
- MRI (magnetic resonance imaging): In some cases, an MRI may be used for a more detailed view, especially if the CT scan results are inconclusive or further information is needed.
X-rays of the skull may also be taken to check for fractures or other abnormalities.
Once diagnosed, the severity of the subdural hematoma and the patient’s overall condition will guide any treatment approach, which may include observation, medication, or surgical intervention, depending on the specific circumstances. Early and accurate diagnosis is essential for managing the subdural hematoma and preventing complications.
How are subdural hematomas treated?
The treatment of subdural hematomas depends on various factors, including the size of the hematoma, the severity of symptoms, and the overall health of the patient. Here are a few common approaches to treating subdural hematomas:
- Observation: Small, asymptomatic subdural hematomas may be managed through close observation. This typically involves monitoring the patient’s neurological status and conducting repeat imaging studies to track any changes in the hematoma size.
- Medication: Corticosteroids or diuretics may be prescribed to reduce inflammation and manage associated symptoms.
- Surgery:
- Burr hole surgery: This involves drilling one or more small holes in the skull to drain the accumulated blood and relieve pressure on the brain. It is a common and less invasive surgical procedure.
- Craniotomy: In more severe cases, a larger surgical opening in the skull may be necessary to remove the hematoma and address any underlying issues.
- Decompressive craniectomy: In cases of significant brain swelling, a portion of the skull may be temporarily removed to allow the brain to expand and reduce pressure. The removed skull piece is usually replaced later through a second surgery.
The choice of treatment depends on factors such as the size and thickness of the hematoma, the patient’s neurological condition, and the underlying causes of the hematoma.
What causes subdural hematomas?
The NHS states, “Subdural hematomas are usually caused by a head injury. Head injuries that cause subdural hematomas are often severe, such as from a car crash, fall or violent assault. Minor bumps to the head can also lead to a subdural hematoma in a few cases.”
Although anyone can develop a subdural hematoma, especially after a head injury, some groups of people may be more at risk. These factors include:
- Age: The majority of chronic subdural hematomas affect people over age 60, and the chances of developing one increase as you age. “This is thought to be because most people’s brains shrink to some degree as they get older. This places the brain’s blood vessels under increased tension, like a stretched rubber band, and means they’re more vulnerable to damage from minor injuries.”
- Alcohol abuse: Misuse of alcohol over a long period can cause the brain to shrink, making it more vulnerable to damage and injuries.
- Blood thinners: Anticoagulant medications may increase the risk of hematoma, because your blood clots less easily and any bleeding in the brain can quickly turn severe.
It’s important to note that while head injuries are a common cause, in some cases, subdural hematomas may also occur spontaneously without a clear traumatic event. Understanding the underlying cause is essential for determining the appropriate treatment and preventative measures. Individuals at risk for head injuries should take precautions to minimize that risk, and those with bleeding disorders should work closely with their healthcare providers to manage their condition.
Recovering from a subdural hematoma
The NHS also reports, “How long it takes to recover varies from person to person. Some people may feel better within a few weeks or months, while others may never make a full recovery even after many years. This will largely depend on how severe the damage to your brain is.”
Patients may experience changes in mood, memory problems, seizures, problems with concentration, speech problems, and weakness in the limbs. There is also the risk that the hematoma can come back after treatment – if any of your symptoms return, like a worsening headache or confusion, talk to a doctor right away.
During the recovery period, you may need various sorts of rehabilitation, including physical therapy, speech and language therapy, and occupational therapy.
If you suffered a traumatic brain injury like a subdural hematoma due to someone else’s negligence, talk to the Charlotte personal injury attorneys at Price, Petho & Associates today. We can help hold the right people accountable and work toward securing you the compensation you deserve for your injuries, pain, and suffering. To schedule a free consultation, please call our office or complete our contact form today. We have offices in Charlotte, Rockingham, and Rutherfordton for your convenience.

Doug Petho is the owner and founder of Price, Petho & Associates. His focus is the litigation of plaintiff’s personal injury suits, and he has successfully tried hundreds of cases to jury verdict involving car accidents, trucking accidents, pedestrian accidents, and slip and fall accidents. Contact his Charlotte office.
